Understanding Wound Care Assessment and Its Clinical Importance
Wound care assessment is a structured clinical process used to evaluate the condition of a wound, determine its stage of healing, and identify factors that may influence recovery. It is a foundational skill in nursing and medical practice because it directly impacts treatment decisions and patient outcomes. Accurate wound evaluation helps clinicians identify complications early and adjust interventions before deterioration occurs. It is applied in hospitals, long-term care facilities, outpatient clinics, and home healthcare environments. The process also supports continuity of care across multidisciplinary teams.
Effective wound care assessment requires attention to detail and consistency in evaluation methods. Clinicians rely on both visual inspection and standardized measurement techniques to ensure accuracy. The assessment provides insight into whether a wound is healing as expected or showing signs of infection or delay. It also helps determine the appropriate type of dressing or intervention needed. Without proper evaluation, treatment plans may become ineffective or even harmful.
This clinical process also plays a role in reducing healthcare costs by preventing complications that require advanced interventions. Patients benefit from faster recovery times when wounds are accurately monitored. It also improves communication between healthcare providers by providing a clear record of wound status over time. As healthcare continues to evolve, structured wound care assessment remains a critical component of patient-centered care.
Core Principles of Wound Healing and Tissue Response
Wound healing is a complex biological process that occurs in a predictable sequence of phases. These phases include hemostasis, inflammation, proliferation, and maturation. Each phase plays a distinct role in repairing damaged tissue and restoring skin integrity. Understanding these stages is essential for accurate wound care assessment and appropriate clinical decision-making.
During the inflammatory phase, the body works to control bleeding and prevent infection. White blood cells migrate to the wound site to remove debris and pathogens. In the proliferative phase, new tissue begins to form, including granulation tissue and new blood vessels. The maturation phase strengthens the repaired tissue over time.
Several factors influence wound healing efficiency, including oxygenation, nutrition, circulation, and immune response. Chronic conditions such as diabetes can slow the healing process significantly. Environmental factors and infection presence also impact recovery. Clinicians must consider all these variables during evaluation.
Proper understanding of tissue response allows healthcare providers to identify deviations from normal healing patterns. This helps guide interventions that support optimal recovery and prevent complications.
Types of Wounds Commonly Encountered in Clinical Practice
Wounds are classified based on their cause, duration, and healing potential. Acute wounds typically result from surgical procedures, trauma, or injuries and are expected to follow a normal healing trajectory. Chronic wounds, on the other hand, fail to progress through the normal healing stages and often require long-term care. These include diabetic foot ulcers, venous leg ulcers, and pressure injuries.
Burn wounds vary in severity depending on depth and tissue involvement. Superficial burns affect only the outer layer of skin, while deeper burns may damage muscles and nerves. Atypical wounds may arise from unusual causes such as autoimmune conditions or malignancies.
Understanding wound classification is essential in wound care assessment because it determines the treatment approach. Each type of wound requires different management strategies and monitoring frequency. Clinicians must also consider wound origin when evaluating risk factors for delayed healing. Proper classification ensures accurate documentation and communication across healthcare teams.
Systematic Approach to Performing a Wound Care Assessment
A structured approach is essential for consistency and accuracy in wound evaluation. The process begins with patient identification and preparation, ensuring comfort and privacy. Clinicians then proceed with visual inspection and measurement of the wound. Standardized techniques are used to record length, width, depth, and overall appearance.
Consistency in method ensures that changes in wound status can be accurately tracked over time. Clinicians often use the same tools and protocols during each assessment to reduce variability. Environmental factors such as lighting and cleanliness also influence evaluation quality. Proper hand hygiene and infection control measures are critical during the process.
A systematic approach includes evaluating surrounding tissue, wound bed condition, and exudate characteristics. This structured method helps ensure no important detail is overlooked. It also supports better communication between healthcare providers involved in patient care.
Patient History Collection and Its Role in Wound Evaluation
Patient history is a critical component of wound care assessment because it provides context for the wound’s development and healing potential. Medical conditions such as diabetes, vascular disease, and immune disorders significantly affect recovery rates. Medication history is also important, as certain drugs can impair healing or increase bleeding risk.
Lifestyle factors play a major role in wound progression. Smoking, poor nutrition, and limited mobility can delay healing significantly. Previous wound occurrences provide insight into recurrence risks and long-term management needs. Understanding these factors allows clinicians to create more effective treatment plans.
A thorough patient history also includes psychosocial considerations. Stress levels, support systems, and access to healthcare resources influence recovery outcomes. Clinicians must take a holistic approach when gathering this information. This ensures that treatment plans address both physical and environmental factors.
Physical Examination of Wounds: What Clinicians Must Observe
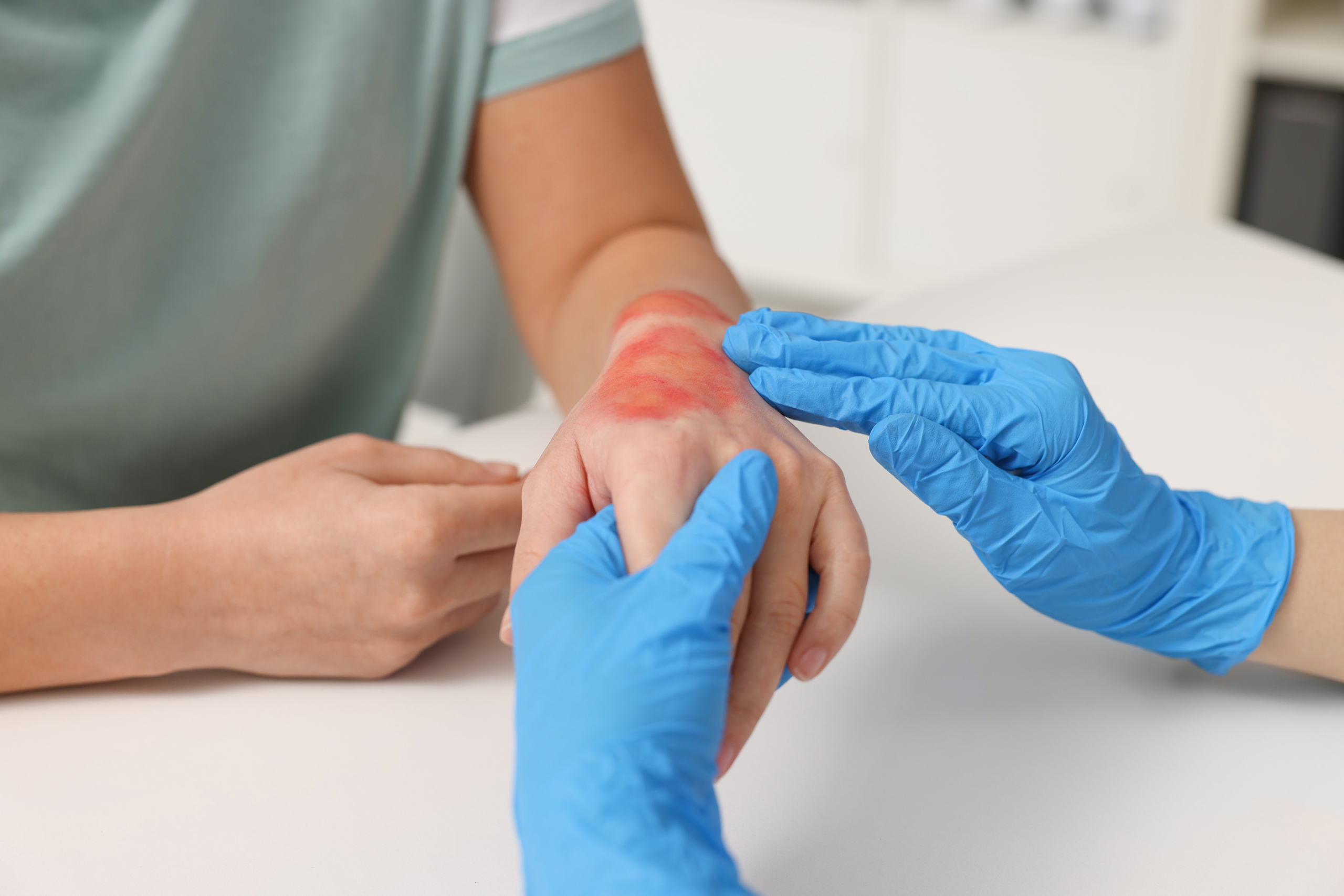
Physical examination is the most direct component of wound care assessment. It involves careful inspection of the wound bed, edges, and surrounding skin. Clinicians assess tissue type to determine healing progress, identifying granulation tissue, slough, or necrotic material. The condition of wound edges provides additional information about healing status.
Measurement is a key part of the physical examination process. Wound dimensions must be recorded accurately and consistently. Surrounding skin is evaluated for signs of irritation, maceration, or discoloration. Exudate is assessed based on quantity, color, and odor.
Key elements observed during physical examination include:
- Wound size and depth measurements
- Type and condition of tissue present
- Presence and characteristics of exudate
- Condition of wound edges and surrounding skin
- Signs of infection or abnormal healing
- Temperature changes around the wound site
- Pain response during examination
These observations provide essential data for determining treatment effectiveness. They also help identify complications early, allowing for timely intervention.
Standardized Tools and Scales Used in Wound Care Assessment
Standardized tools are essential for ensuring consistency in wound evaluation. They provide structured frameworks for measuring wound severity and tracking healing progress. Common tools include the Braden Scale, PUSH Tool, and Bates-Jensen Wound Assessment Tool. These systems help reduce subjectivity in clinical evaluation.
Digital technologies are increasingly being used to enhance accuracy. Imaging software and measurement apps allow clinicians to capture precise wound dimensions. These tools also enable long-term tracking and comparison of wound progression. Standardization improves communication between healthcare providers.
These tools support clinical decision-making by providing measurable data. They also help prioritize patient care based on wound severity. Proper use of standardized systems enhances overall treatment effectiveness.
Documentation Practices for Accurate Wound Tracking
Accurate documentation is a vital part of wound care assessment. It ensures continuity of care and provides a record of wound progression over time. Clinical notes must include detailed descriptions of wound characteristics and measurements. Photographic documentation is often used to supplement written records.
Electronic health records have improved accessibility and organization of wound data. They allow multiple healthcare providers to access updated information easily. Proper documentation also supports legal and ethical compliance in clinical practice.
Consistency in documentation ensures reliable tracking of healing progress. It also improves communication between multidisciplinary teams involved in patient care.
Identifying Infection and Complications During Wound Evaluation
Infection is one of the most serious complications in wound care. Early detection is critical to prevent systemic spread and further tissue damage. Signs of infection include redness, swelling, increased pain, and abnormal discharge. Foul odor and delayed healing may also indicate infection.
Systemic symptoms such as fever and fatigue suggest more advanced infection. Clinicians must differentiate between normal inflammation and infection. This distinction is essential for appropriate treatment decisions.
Complications may also include necrosis, abscess formation, and cellulitis. Early identification through wound care assessment improves patient outcomes significantly.
Pain Assessment in Patients With Acute and Chronic Wounds
Pain is a significant factor in wound care assessment. It affects patient comfort and can influence healing outcomes. Clinicians use standardized pain scales to measure intensity and frequency. Pain may indicate infection, tissue damage, or inadequate treatment.
Pain management strategies are often integrated into wound care plans. Addressing pain improves patient compliance and overall recovery experience. Continuous evaluation ensures that treatment remains effective and tolerable.
Role of Nutrition and Comorbidities in Wound Healing Progress
Nutrition plays a vital role in tissue repair and regeneration. Proteins, vitamins, and minerals are essential for wound healing. Poor nutritional status can delay recovery significantly. Hydration also supports cellular function and tissue repair.
Comorbid conditions such as diabetes and vascular disease impair circulation and immune response. These conditions must be considered during wound care assessment. Proper management of underlying diseases improves healing outcomes.
Advanced Diagnostics and Imaging in Complex Wound Assessment
Advanced diagnostic tools enhance accuracy in complex cases. Imaging technologies such as ultrasound and MRI provide detailed views of underlying tissue damage. Oxygen measurement devices help assess tissue viability.
These tools are particularly useful for chronic or non-healing wounds. They allow clinicians to identify hidden complications that are not visible during physical examination. Advanced diagnostics support more precise treatment planning.
Interdisciplinary Collaboration in Wound Management
Wound management often requires collaboration between multiple healthcare professionals. Nurses, physicians, dietitians, and specialists contribute to patient care. Effective communication ensures consistent treatment approaches.
Each professional brings unique expertise to the wound care assessment process. Collaboration improves treatment efficiency and patient outcomes. Coordinated care reduces the risk of complications and enhances recovery.
Treatment Planning Based on Wound Care Assessment Findings
Treatment planning is directly guided by wound evaluation results. Clinicians select dressings and therapies based on wound type and severity. Debridement may be necessary for removing necrotic tissue.
Regular reassessment ensures that treatment remains effective. Adjustments are made based on healing progress and patient response. Personalized care plans improve recovery outcomes.
Patient Education and Self-Care Strategies for Wound Management
Patient education is essential for successful wound care. Patients must understand proper wound hygiene techniques and dressing changes. Education improves adherence to treatment plans.
Patients are also taught to recognize signs of infection or deterioration. Lifestyle modifications such as improved nutrition and smoking cessation support healing. Empowering patients enhances long-term outcomes.
Common Challenges in Wound Care Assessment and How to Address Them
Challenges in wound care assessment include inconsistent evaluation techniques and limited resources. Chronic wounds may be difficult to assess due to complexity. Patient non-compliance can also hinder progress.
Standardized training and protocols help reduce variability. Improved communication and education address many of these challenges. Resource optimization enhances care delivery.
Emerging Trends and Innovations in Wound Assessment Technology
Technology is transforming wound care assessment practices. Artificial intelligence tools assist in analyzing wound images and predicting healing outcomes. Smart dressings provide real-time monitoring of wound conditions.
Mobile applications allow remote tracking of wound progress. These innovations improve accuracy and accessibility of care. Future developments will continue to enhance clinical efficiency.
Frequently Asked Questions
What is wound care assessment?
It is the clinical evaluation of a wound to determine its condition, healing stage, and treatment needs.
Why is wound care assessment important?
It helps guide treatment decisions and prevents complications such as infection and delayed healing.
How often should wounds be assessed?
Frequency depends on wound severity, but regular monitoring is essential for chronic wounds.
What tools are used in wound care assessment?
Common tools include the Braden Scale, PUSH Tool, and digital imaging systems.
What signs indicate wound infection?
Redness, swelling, pain, odor, and abnormal discharge are common indicators.
Takeaway
Wound care assessment is a structured and essential clinical practice that ensures accurate evaluation, supports effective treatment planning, and improves healing outcomes.