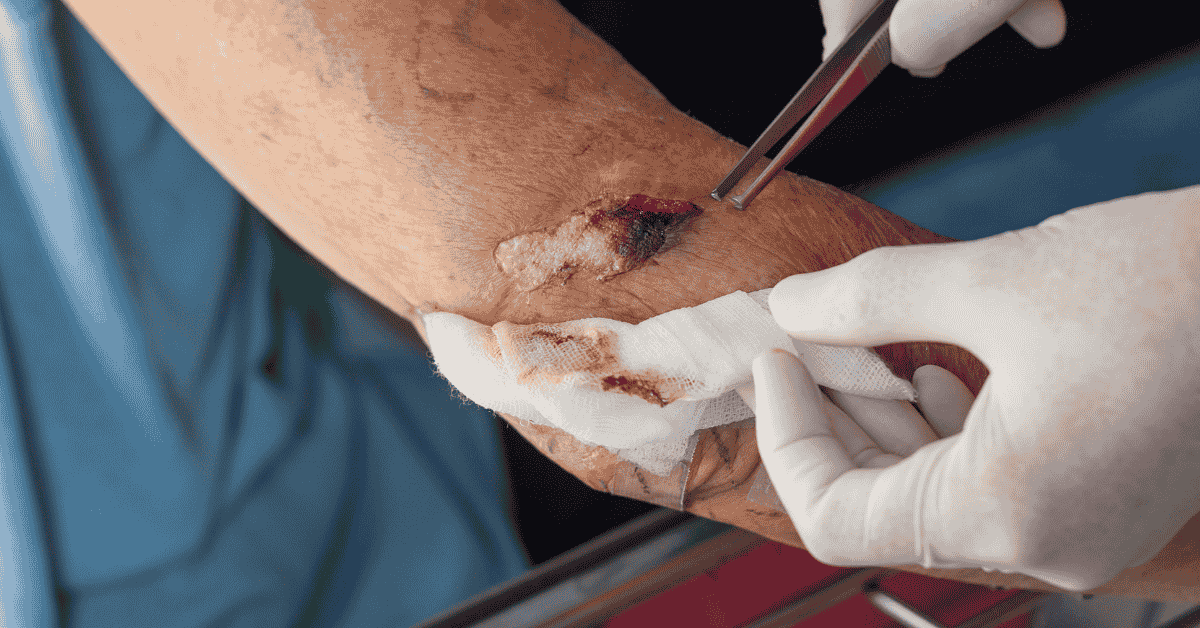
Understanding Emergency Sever Wound Surgery in Critical Trauma Care
Emergency sever wound surgery refers to urgent surgical intervention performed on deep, life-threatening injuries that involve extensive damage to skin, muscle, blood vessels, nerves, or bone. This type of surgery is required when a wound is too severe for basic medical treatment and poses immediate risks such as massive bleeding, infection, or loss of limb function. In clinical practice, sever wound surgery is often performed in trauma units where rapid decision-making is essential to preserve life and tissue viability. These injuries are commonly caused by road accidents, industrial incidents, falls from height, or violent trauma. The surgical goal is to stabilize the patient, remove damaged tissue, and restore structural integrity as quickly as possible. Medical teams treat these cases as time-sensitive emergencies because delays can significantly worsen outcomes. Every step of care is coordinated to minimize complications and maximize recovery potential.
Sever wound surgery also involves evaluating both visible and hidden damage, which may include internal bleeding or organ injury. Surgeons must act quickly while maintaining precision to avoid further harm. The complexity of these cases often requires collaboration between trauma surgeons, orthopedic specialists, and vascular surgeons. Patients undergoing this procedure often require intensive post-operative monitoring in a hospital setting. The importance of emergency sever wound surgery lies in its ability to prevent permanent disability and save lives in critical situations.
Major Types of Injuries Requiring Sever Wound Surgery
Sever wound surgery is necessary for a wide range of traumatic injuries that cannot heal without surgical intervention. Deep lacerations are one of the most common conditions, where the skin and underlying tissues are severely cut, often exposing muscles or bone. These injuries usually involve heavy bleeding and require immediate closure to prevent infection. Crush injuries are another serious category, typically caused by heavy pressure or impact that damages tissues, blood vessels, and bone structures simultaneously.
Avulsion injuries occur when skin or tissue is forcibly torn away from the body, creating irregular and complex wounds that require reconstructive techniques. Penetrating injuries, such as those caused by sharp objects or high-impact trauma, may damage internal organs and require exploratory surgery. Severe burn injuries also fall under this category, especially when deep layers of skin are destroyed and require grafting procedures. Each type of injury presents unique surgical challenges that require specialized treatment planning. The severity of the wound determines whether multiple surgical stages are required for full recovery.
Emergency Response Before Sever Wound Surgery
Immediate emergency care is critical before performing sever wound surgery, as it significantly affects patient survival and recovery outcomes. The first priority is controlling bleeding through direct pressure, compression dressings, or tourniquet application when necessary. Stabilizing vital signs such as heart rate, blood pressure, and oxygen levels is essential to prevent shock. Emergency responders also focus on keeping the wound as clean as possible to reduce contamination risks.
Once stabilized, patients are quickly transported to trauma centers equipped for advanced surgical intervention. Diagnostic imaging, including X-rays, CT scans, and ultrasound, helps identify internal injuries that are not visible externally. These assessments allow medical teams to determine the urgency and complexity of surgical procedures. Pain management is also initiated during this stage to improve patient stability. Proper emergency response significantly increases the success rate of sever wound surgery.
Diagnostic Evaluation for Sever Wound Surgery
Accurate diagnosis is a crucial step before performing sever wound surgery, as it guides surgical planning and treatment decisions. Physicians begin with a physical examination to assess wound depth, tissue damage, and bleeding severity. Circulation checks are performed to determine whether blood flow is compromised in the affected area. In cases of severe trauma, hidden injuries such as internal bleeding or organ damage must also be ruled out.
Advanced imaging techniques provide detailed insights into the extent of injury. CT scans help identify internal fractures or organ involvement, while ultrasound is useful for detecting fluid buildup or vascular damage. Laboratory tests may also be conducted to assess infection risk or blood loss. Tissue viability evaluations help determine which areas can be saved and which must be removed. A thorough diagnostic process ensures that sever wound surgery is performed with precision and effectiveness.
Surgical Procedures Used in Sever Wound Surgery
Sever wound surgery involves a combination of surgical techniques tailored to the severity of the injury. Debridement is one of the most important procedures, where dead or infected tissue is removed to promote healing and prevent infection. This step is essential for creating a clean surgical environment. Wound closure techniques such as sutures, staples, or medical adhesives are used depending on wound characteristics.
Skin grafting is often required when large areas of skin are lost, involving the transfer of healthy skin from another part of the body or the use of synthetic substitutes. Reconstructive surgery plays a major role in restoring damaged muscles, tendons, and structural tissues. Microsurgery techniques allow surgeons to repair small blood vessels and nerves with high precision. These procedures work together to restore both function and appearance. Sever wound surgery often requires multiple stages to achieve optimal results.
Anesthesia and Pain Control in Surgery
Anesthesia is a critical component of sever wound surgery, ensuring that patients remain pain-free and stable during procedures. Depending on the complexity of the injury, local, regional, or general anesthesia may be used. Local anesthesia numbs a small area, while regional anesthesia blocks sensation in larger body regions. General anesthesia is used for complex surgeries requiring full unconsciousness.
Pain management continues after surgery through medications that reduce discomfort and inflammation. Medical teams closely monitor patient responses to ensure safety and comfort. Proper anesthesia use also helps surgeons perform procedures with greater precision. Pain control plays a major role in improving recovery outcomes. Effective management of anesthesia is essential for successful sever wound surgery.
Infection Prevention and Wound Care Management
Infection control is one of the most important aspects of sever wound surgery due to the high risk of bacterial contamination. Surgical environments are maintained under strict sterilization protocols to ensure patient safety. Antibiotics are often administered before and after surgery to prevent infection development. Proper wound cleaning and dressing changes are essential during recovery.
Healthcare professionals closely monitor wounds for signs of infection such as redness, swelling, or unusual discharge. Early detection allows for immediate treatment and prevents complications. Sterile techniques are used throughout the surgical process to reduce contamination risks. Infection prevention significantly improves healing outcomes. This stage is critical for long-term recovery success.
Recovery Process After Sever Wound Surgery
Recovery following sever wound surgery is a gradual process that requires medical supervision and patient commitment. Immediately after surgery, patients are monitored to ensure stable vital signs and proper wound healing. Dressings are changed regularly to maintain cleanliness and support healing. Pain management is continued to ensure patient comfort during recovery.
Rehabilitation therapy may be required to restore movement and strength in affected areas. Nutritional support plays a vital role in tissue repair, with emphasis on protein and essential vitamins. Scar management treatments such as topical creams or laser therapy may be recommended. Recovery timelines vary depending on injury severity and surgical complexity. Consistent follow-up care ensures optimal healing progress.
Possible Complications After Surgery
Although sever wound surgery is highly effective, complications may still occur during recovery. Infection remains one of the most common risks, particularly in deep or contaminated wounds. Delayed healing can occur due to poor circulation or underlying health conditions. Tissue necrosis may develop if damaged areas do not receive adequate blood supply.
Nerve damage is another possible complication that may affect sensation or mobility. Blood clots can also form and require immediate medical attention. Surgeons take preventive measures, but continuous monitoring is essential. Early detection of complications improves treatment success. Awareness of these risks helps patients stay alert during recovery.
Long-Term Recovery and Outcomes
Long-term outcomes of sever wound surgery depend on injury severity, surgical precision, and rehabilitation quality. Many patients regain significant function and mobility after proper treatment and recovery. However, some may experience lasting effects such as scarring or reduced flexibility. Reconstructive procedures can improve both physical appearance and functional ability.
Psychological recovery is also important, as traumatic injuries can affect emotional well-being. Ongoing medical follow-ups help ensure that healing continues as expected. Advances in surgical techniques have improved long-term success rates significantly. Patients are encouraged to maintain healthy habits to support full recovery. Each case has unique healing potential based on individual circumstances.
Advances in Sever Wound Surgery Technology
Modern advancements have significantly improved the effectiveness of sever wound surgery. Robotic-assisted surgical systems allow for greater precision and control during complex procedures. 3D imaging technology enables surgeons to visualize injuries in detail before operating. Bioengineered skin substitutes are now widely used for large or complex wounds.
Regenerative medicine is also transforming tissue repair and healing processes. Advanced surgical materials improve wound closure strength and flexibility. These innovations have reduced recovery times and improved patient outcomes. Continuous research continues to enhance surgical techniques. Technology plays a key role in improving survival and recovery rates.
Preventive Measures for Severe Injuries
Preventing injuries that require sever wound surgery is essential for reducing trauma cases. Workplace safety measures such as protective gear can significantly lower accident risks. Road safety practices, including seatbelt use and defensive driving, help prevent severe injuries. Sports participants should use proper equipment and training techniques.
Home safety awareness also plays a role in preventing accidents such as falls or cuts. Public education on safety practices helps reduce trauma-related incidents. Employers and communities must promote consistent safety standards. Prevention remains the most effective strategy for avoiding severe injuries. Awareness and caution are key to reducing risks.
When Immediate Medical Attention Is Needed
Immediate medical attention is necessary when severe wounds occur with uncontrolled bleeding or exposed internal structures. Deep wounds involving muscle or bone require urgent surgical evaluation. Symptoms such as dizziness, rapid heartbeat, or confusion may indicate shock. Severe pain or numbness can signal nerve or tissue damage.
Foreign objects embedded in wounds should not be removed without medical supervision. Delaying treatment can significantly increase risks and complications. Emergency care facilities are equipped to handle these critical situations. Quick medical response improves survival and recovery outcomes. Recognizing warning signs is essential for timely intervention.
Frequently Asked Questions (FAQ)
What is sever wound surgery?
Sever wound surgery is a medical procedure used to treat deep and complex traumatic injuries that cannot heal on their own. It involves cleaning, repairing, and reconstructing damaged tissues. The goal is to restore function and prevent infection. It is commonly performed in emergency trauma settings. Surgeons may use multiple techniques depending on injury severity. It often requires specialized medical teams. This surgery is critical in saving lives and preventing disability.
How long does recovery take after sever wound surgery?
Recovery time varies depending on injury severity and surgical complexity. Some patients recover within weeks, while others may require months of rehabilitation. Physical therapy is often necessary for full recovery. Healing also depends on overall health and medical compliance. Complications can extend recovery time. Regular follow-ups are essential. Each patient’s recovery process is unique.
Is sever wound surgery painful?
Patients do not feel pain during surgery due to anesthesia. After surgery, some discomfort is normal as the body heals. Pain is managed with medications prescribed by doctors. The intensity of pain depends on the injury and procedure. Most patients experience gradual improvement. Medical teams closely monitor pain levels. Proper care helps reduce discomfort effectively.
What are the risks of sever wound surgery?
Risks include infection, delayed healing, nerve damage, and blood clots. Some patients may require additional surgeries. Tissue complications may also occur depending on injury severity. Medical teams take preventive measures to reduce risks. Continuous monitoring helps detect problems early. Patient health conditions also influence outcomes. Despite risks, surgery is often necessary for survival and recovery.
Can severe wounds fully heal after surgery?
Many severe wounds heal significantly, but full recovery depends on injury severity. Some patients may have scarring or minor limitations. Reconstructive surgery improves function and appearance. Rehabilitation plays a major role in recovery success. Healing potential varies per individual. Medical advancements have improved outcomes greatly. Each case requires personalized treatment.
What is the difference between stitching and reconstructive surgery?
Stitching is used for simple wound closure, while reconstructive surgery is used for complex injuries. Reconstructive procedures restore damaged tissues, muscles, or structures. Stitching is a basic form of wound repair. Severe injuries often require advanced surgical techniques. Reconstruction may involve grafts or microsurgery. The complexity of the injury determines the method used. Both aim to promote healing.
How is infection prevented after surgery?
Infection prevention involves antibiotics, sterile procedures, and proper wound care. Dressings must be changed regularly. Patients must follow medical instructions carefully. Hospitals maintain strict hygiene standards. Early detection of infection signs is essential. Clean environments reduce contamination risks. Proper care ensures better healing outcomes.
Are skin grafts permanent?
Skin grafts are generally long-lasting and integrate with surrounding tissue. They provide permanent coverage in most cases. Some changes in texture or appearance may occur. Proper care improves durability. Additional procedures may sometimes be needed. Grafts help restore protection and function. They are widely used in severe wound treatment.
Takeaway
Sever wound surgery is a critical medical procedure designed to treat life-threatening traumatic injuries that involve deep tissue damage. It combines emergency response, advanced surgical techniques, and long-term rehabilitation to restore function and improve patient outcomes. Early intervention, proper surgical care, and consistent recovery support significantly increase healing success.