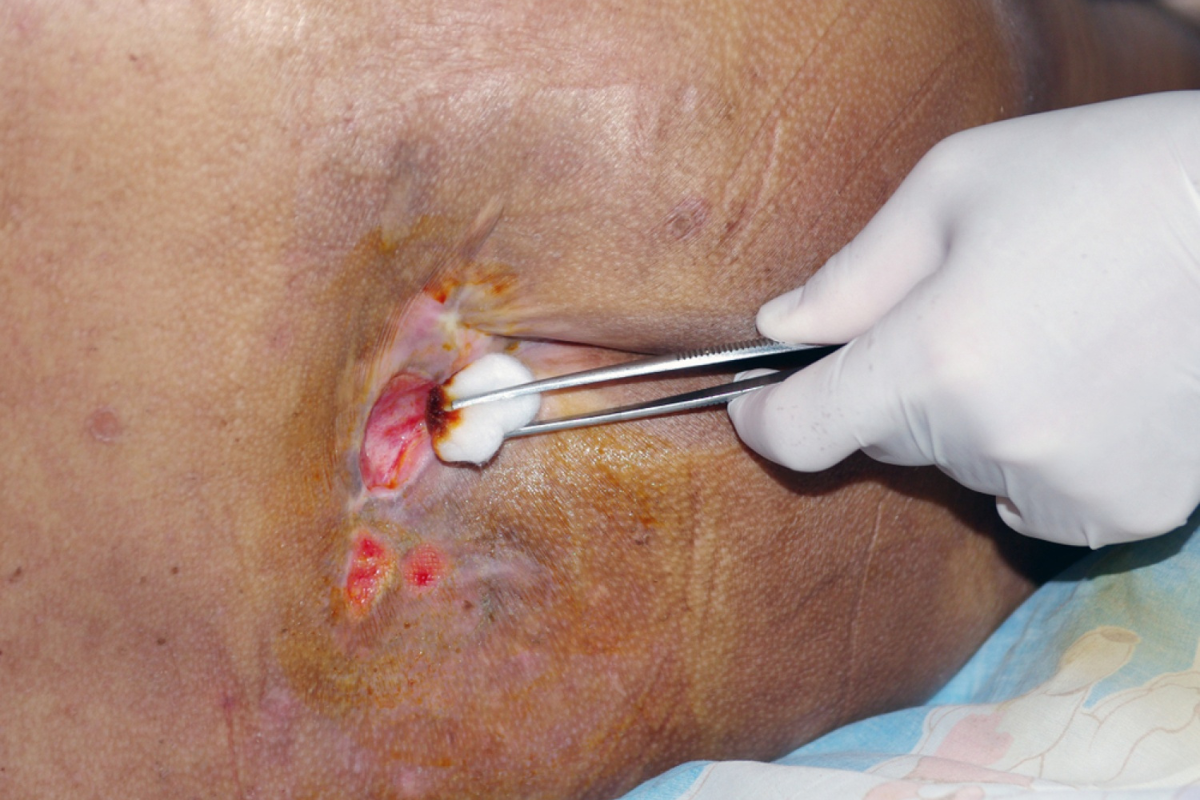
Understanding Decubitus Ulcers and Their Impact on Patient Health
Decubitus ulcer treatment is an essential part of care for individuals who experience limited mobility or prolonged pressure on the skin. These ulcers form when constant pressure restricts blood flow to specific areas of the body, commonly the hips, heels, tailbone, and shoulders. Without adequate circulation, skin and underlying tissues begin to deteriorate, leading to open wounds. Many patients experience discomfort, pain, and reduced mobility as ulcers progress. When left untreated, these wounds can become infected and cause serious medical complications. Effective decubitus ulcer treatment focuses not only on wound healing but also on improving patient comfort and daily function. Understanding how these ulcers affect overall health highlights the importance of timely and consistent care.
Contributing Factors That Shape Decubitus Ulcer Treatment Plans
Several contributing factors influence how decubitus ulcer treatment is planned and carried out. Immobility is the most significant risk, especially among bedridden patients and wheelchair users. Poor circulation reduces oxygen delivery to tissues, slowing the body’s natural healing response. Inadequate nutrition weakens the skin and limits its ability to regenerate. Excess moisture from sweat or incontinence increases skin breakdown and irritation. Chronic illnesses such as diabetes further complicate healing by impairing blood flow and immune response. Aging skin is thinner and more fragile, increasing vulnerability to pressure damage. Addressing these factors allows healthcare providers to customize treatment plans that support long term healing.
Recognizing Ulcer Severity and Matching the Right Treatment
Decubitus ulcer treatment must be adapted to the severity of the wound. Early stage ulcers may appear as persistent redness or skin discoloration that does not fade with pressure relief. Moderate ulcers involve partial skin loss and may present as blisters or shallow open wounds. Advanced ulcers extend deeper into muscle or connective tissue and require intensive medical care. The most severe ulcers expose bone or tendons and often lead to complications if not managed promptly. Some wounds are difficult to classify due to dead tissue covering the surface. Accurate evaluation ensures that treatment matches the wound’s depth and condition. Proper staging helps prevent progression and supports effective healing.
Clinical Evaluation and Monitoring for Treatment Accuracy
Thorough evaluation is a cornerstone of successful decubitus ulcer treatment. Healthcare providers examine the wound’s size, depth, drainage, and surrounding skin condition. Signs of infection such as swelling, warmth, or unusual odor are carefully monitored. Pain levels provide insight into tissue damage and patient comfort. In certain cases, diagnostic tests may be ordered to assess deeper tissue involvement. Ongoing monitoring allows clinicians to track healing progress and make necessary adjustments. Documentation ensures consistency across care teams. Accurate assessment helps maintain effective and responsive treatment.
Standard Medical Approaches Used in Decubitus Ulcer Treatment
Decubitus ulcer treatment relies on several standard medical strategies that work together to promote healing. Pressure relief is the foundation of care and is achieved through regular repositioning. Wound cleansing removes debris and reduces bacterial growth. Dressings are selected based on wound condition to maintain moisture balance. Debridement may be used to remove damaged tissue that delays healing. Pain management improves patient comfort and cooperation with care routines. Consistency is essential to achieving positive results.
Key Components That Support Healing
• Scheduled repositioning to reduce prolonged pressure
• Use of pressure relieving mattresses and cushions
• Proper wound cleaning and dressing application
• Removal of dead or infected tissue when required
• Supportive pain management and comfort measures
These components work together to create an optimal healing environment.
Advanced Treatment Options for Complex Ulcers
Some cases of decubitus ulcer treatment require advanced medical interventions. Negative pressure wound therapy helps remove excess fluid and encourages tissue regeneration. Specialized dressings containing growth promoting materials may be used for difficult wounds. Oxygen based therapies improve circulation in damaged tissues. Surgical procedures may be considered when wounds do not respond to conservative care. Advanced treatments are typically guided by wound care specialists. Multidisciplinary collaboration ensures comprehensive management. These options improve outcomes for severe or chronic ulcers.
Nutritional Support as a Core Element of Healing
Nutrition plays a vital role in effective decubitus ulcer treatment. Adequate protein intake supports tissue repair and immune function. Vitamins and minerals assist with collagen formation and wound closure. Proper hydration maintains skin elasticity and circulation. Patients with nutritional deficiencies often experience delayed healing. Dietitians help design meal plans that support recovery. Regular nutritional assessments ensure ongoing effectiveness. Balanced nutrition strengthens the body’s ability to heal and resist infection.
Managing Infection Risks During Treatment
Infection control is a critical focus in decubitus ulcer treatment. Open wounds provide an opportunity for bacteria to enter the body. Proper hygiene and clean dressing techniques reduce contamination. Early recognition of infection allows for prompt medical intervention. Antibiotic therapy may be necessary in some cases. Caregivers must understand warning signs such as increased redness or drainage. Preventing infection protects both the wound and overall health. Vigilant care reduces the risk of serious complications.
Preventive Strategies That Enhance Treatment Outcomes
Prevention supports long term success in decubitus ulcer treatment. Pressure redistribution devices reduce stress on vulnerable areas. Routine skin inspections help detect early signs of damage. Maintaining mobility improves circulation and tissue health. Education empowers patients and caregivers to take preventive action. Individualized care plans address specific risk factors. Preventive measures reduce recurrence rates. Proactive care improves quality of life and treatment success.
Home Based Care and Caregiver Responsibilities
Home care plays an important role in ongoing decubitus ulcer treatment. Caregivers must be trained in proper wound care techniques. Maintaining a clean environment supports healing. Repositioning schedules must be followed consistently. Monitoring wound changes ensures timely medical attention. Emotional support helps patients cope with long recovery periods. Collaboration with healthcare providers strengthens care continuity. Informed caregivers significantly improve treatment outcomes.
Common Challenges and Practical Solutions in Treatment
Decubitus ulcer treatment often presents challenges that require patience and adaptability. Slow healing may result from underlying medical conditions. Discomfort can limit patient cooperation. Access to specialized equipment may be restricted. Recurrent ulcers indicate a need for reassessment. Team based care improves problem solving. Clear communication ensures coordinated efforts. Addressing challenges leads to better long term results.
Frequently Asked Questions
What is the primary goal of decubitus ulcer treatment?
The primary goal is to promote wound healing while preventing infection and further skin damage. Treatment also aims to improve comfort and mobility.
How soon should treatment begin after an ulcer appears?
Treatment should begin as soon as signs of skin breakdown are detected. Early care prevents progression and complications.
Are all decubitus ulcers treated the same way?
Treatment varies based on wound severity, patient health, and risk factors. Personalized care plans are most effective.
Can pressure ulcers return after healing?
Yes, recurrence is possible if preventive measures are not maintained. Ongoing care and monitoring reduce this risk.
When should medical attention be sought?
Medical attention is needed if the wound worsens, shows signs of infection, or does not improve with care.
Takeaway
Decubitus ulcer treatment requires dedication, consistency, and a comprehensive care approach that prioritizes both healing and prevention. With proper medical guidance, nutritional support, and attentive caregiving, patients can achieve better outcomes and maintain healthier skin over time.